Edward Pierce's Miracle: How a Broadway Set Designer Beat Covid and Made Medical History
Pierce is the first American to receive a placental cell transplant to fight the insidious virus that left him on a ventilator for five weeks.
Edward Pierce is a busy man. A highly sought-after scenic designer and design adapter, Pierce earned a Tony nomination for the 2018 revival of Angels in America and serves as the global design supervisor for Wicked, to name but two entries in a sprawling list of credits.
In late February, Pierce had designed To Kill a Mockingbird at Madison Square Garden, and he was in the process of adapting Miriam Buether's Broadway set for the upcoming national tour. A few weeks later, he'd be on a ventilator in a medically induced coma.
Pierce is one of the more than 2.4 million people in the United States to contract the coronavirus, and one of the thousands of New Jersey residents to require a ventilator in the hopes of survival (as we've learned, though, once you're on one, you don't usually come off). He was under sedation for a total of five weeks.
In that time, Pierce made medical history. He was the first American recipient of something called a placental cell transplant, created by a pioneering Israeli company called Pluristem, in order to fight the insidious virus. (In short, you are injected with a certain kind of cell from a placenta that can stimulate and regulate the immune system once it goes into the overdrive caused by the virus.)
Pierce calls this treatment a true miracle — he went from near death to leaving the hospital in short order. And he's happy to share his story.

(© David Gordon)
This interview has been lightly condensed and edited for clarity.
When did you first get sick?
On March 9, which was a Monday, I woke up with normal flu-like symptoms. I called the doctor and he prescribed a five-day regime of Tamiflu to get me over it. At that point, it was very early in Covid and there really wasn't a sense of urgency to get to a hospital. By the end of the week, I was getting worse. I was pretty much laying prone on the sofa, hard to breathe. I got through the weekend, but come Monday morning, the doctor was like, "You've got to get to the hospital."
I headed to Holy Name Medical Center near where we live in Teaneck, New Jersey, and right away, my oxygen level was dangerously low. I quickly said goodbye to my wife, who had dropped me off, and I was admitted instantaneously into an isolated room within the ER, where they started treating me as if I was positive for Covid. The infectious disease physician, Dr. Benjamin De La Rosa, started me on the malaria drug, which knocked me out and had quite an effect on my digestive system. I had pneumonia, so they had me on assisted oxygen. By the Thursday of that week, they brought me into a regular isolated Covid room and I really couldn't make it through the night without my oxygen dipping low.
The next morning, they came in and said that the only way for me to get my oxygen level back up was to let my body rest and to put me into a medically induced coma and get me on a ventilator.
What goes through your head when you hear that?
It was super scary thinking that I'd be knocked out and not have any idea what was going on. I couldn't have any visitors, so I was Facetiming my wife and literally expressing all of these same thoughts to her, up to the point when they were getting ready to put the mask over my face. I said I'll see her later and that was that.
I knew, honestly, that I had to do this, because I knew that oxygen alone was not getting me better. I could see in the eyes of the pulmonologist a level of trust and that this was what we've got to do and succumbed to what the medical experts were advising.
And the next thing I know, I'm waking up and someone tells me that I had been on a ventilator for five weeks.
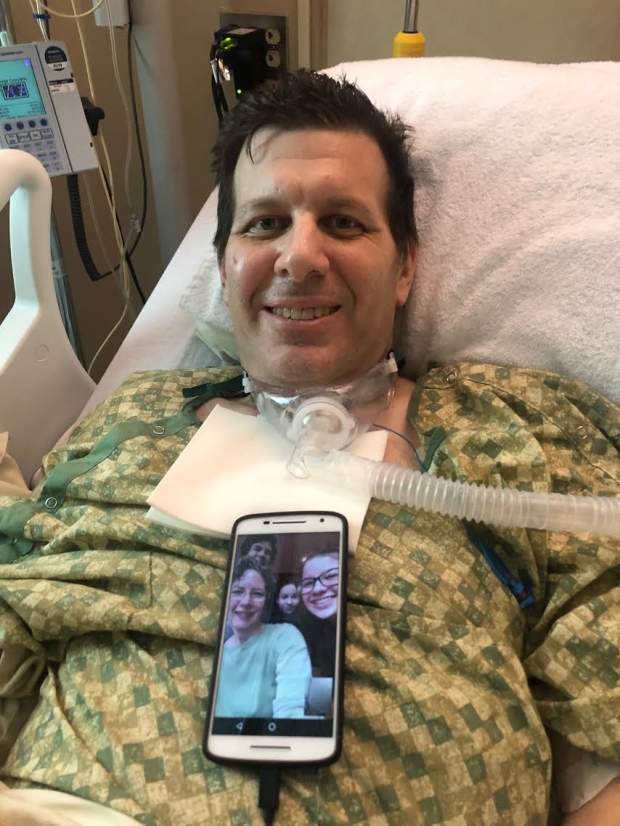
(© Yasmeen Al-Shehab, Holy Name nurse)
It was the experimental placental cell treatment that made the difference?
Honestly, that was our little miracle. They had tried other strategies while I was on the ventilator, one after the next, that didn't do any good. I was on a trial for Remdesivir after the malaria drug didn't seem to pan out and I'd have a couple good days followed by several bad days. But Holy Name Medical Center has a clinical research facility, and one of the doctors, Dr. Ravit Barkama, had been working with the Israeli company Pluristem, using their placental cell treatment for other kinds of patients in the past. She had recently been in Israel meeting with the CEO and they were brainstorming that it might be possible that this treatment could be used for Covid patents.
They approached Pluristem about Holy Name being the first hospital in the state to try it out, and they were a little hesitant but she was very persuasive. That had achieved recognition from the FDA for "compassionate use," to have one US patient do the trial. There were several at Holy Name who were potential candidates, but I'm told they were not as far in the hole as I was and they'd survive on their own with out it. Luckily, they did.
They rushed the placenta cells from Maryland on Friday. On Saturday, they administered 15 shots in various muscles in my arms and legs. From that day, it was all steps forward. Fever dropped away, lungs got more clear, and they started easing me off the ventilator. They reduced the sedation until I was awake.
What happened after?
I left the hospital on Thursday, April 30. I moved out of the ICU the Friday before, and by Monday morning, they started taking out catheters and feeding tubes and eventually the trach tube. They started me on speech therapy and they put me on pureed food, and by the following day, I graduated to real food. By Wednesday, I was on a walker and started moving forward. Come Thursday morning, I was itching to get out of there.
We had come to the conclusion that it would be best for me to transition through Kessler, a local rehab center, to take a little bit of the burden off of going directly home. So much had happened — I went from waking up to coming home — and the house wasn't ready for me and I needed a little more opportunity to strengthen my muscles. The five days I spent was the perfect solution. I still had medical care and got into their rehab gym to learn how to walk upstairs and how to properly walk with a cane, and gain some strength and confidence. I came home the following Wednesday.

(© Jeff Rhode/Holy Name Medical Center)
How are you now, more than three months since?
I think I'm doing great. The first couple weeks I had in-home nursing and physical and occupational therapy care. I quickly graduated from that and continue my physical and occupational therapy at the outpatient facility at Holy Name. That's been wonderful. It gives great structure to my day and I'm exercising more than I ever have in my life.
I lost 35 pounds being on the ventilator that long, most of it muscle mass and strength. Because of the way I was positioned at various times in the ICU, I had several pinched nerves and muscles that have taken a little bit longer to rehabilitate, nothing that anyone thinks is permanent damage, and my strength and energy are building every day.
I'm mentally acute and getting back into communicating with colleagues. I'm very active in United Scenic Artists, which is the union that works with designers, and have been very active in the last few weeks helping the organization get back on its feet and plan the safety protocols as television, film, and live performance get back together again. It's been great to reconnect with colleagues. The Broadway community, as you know, is one big family. You keep adding to that pile and it's wonderful to hear from so many people. Everyone looks to this miraculous story that I share and it brings a little bit of hope and inspiration.
How does it feel to have "made medical history"? Do you think about that?
I do think about that. Each show we do on Broadway is unique and special and a one-off opportunity. If we do something really great, we become a hit. When you become a hit, you get an opportunity to replicate the work that you've done. I've had the extreme honor to be associated with Wicked for 17 years, since the very beginning. We've had the pleasure of being able to re-create our creative work around the world and share it for many, many years.
I see that experience. By trying a medical procedure that is as risky as trying to put on a Broadway production, where it's truly a one-off opportunity, and yet, it was successful, it provides hope that whatever worked for me could be replicated and work for others. I'm so hopeful that the trial is well-reported and that other doctors share this success and pass it around in their network, so others who are suffering the same way I was will be able to try this Pluristem procedure. Perhaps it will do such miraculous work for them as it did for me.

(© Jeff Rhode/Holy Name Medical Center)







